Early detection of eye disease prevents vision loss.
Our family-owned optometry clinic is equipped with world class eye care technologies that promote the early detection and treatment of eye diseases that cause irreversible vision loss. Visit the optometrists and opticians at our Edmonton clinic today and you will see how personalized eye care enables you to be your very best.
Schedule An Exam View Our Services Our Optometrists
(780) 473-6123
Common Eye Conditions, Diseases, & Disorders
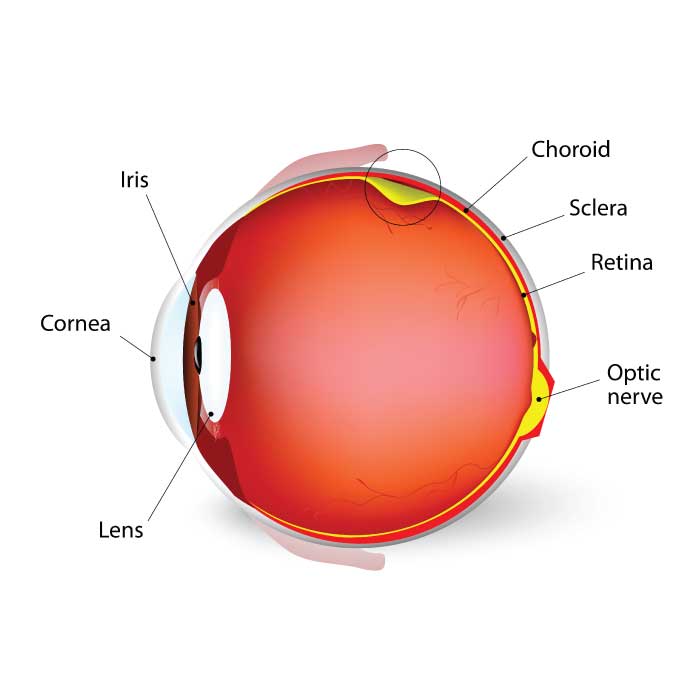
Vision impairment or loss can be caused by eye problems that are hereditary, by conditions that develop later in life, or by infections or environmental factors. Below, is a list of common eye conditions, diseases, and disorders. Along with the provided diagrams we hope this list provides you with a better understanding of the various conditions, diseases, and disorders that can impact your vision and ocular health.
Age-related macular degeneration, glaucoma, cataracts, diabetic retinopathy, and dry eye syndrome are some of the most common eye diseases and disorders. For more information on these eye conditions and others, please ask your optometrist or visit the Canadian National Institute for the Blind (CNIB), Canadian Association of Optometrists, or Alberta Association of Optometrists websites.
Glaucoma
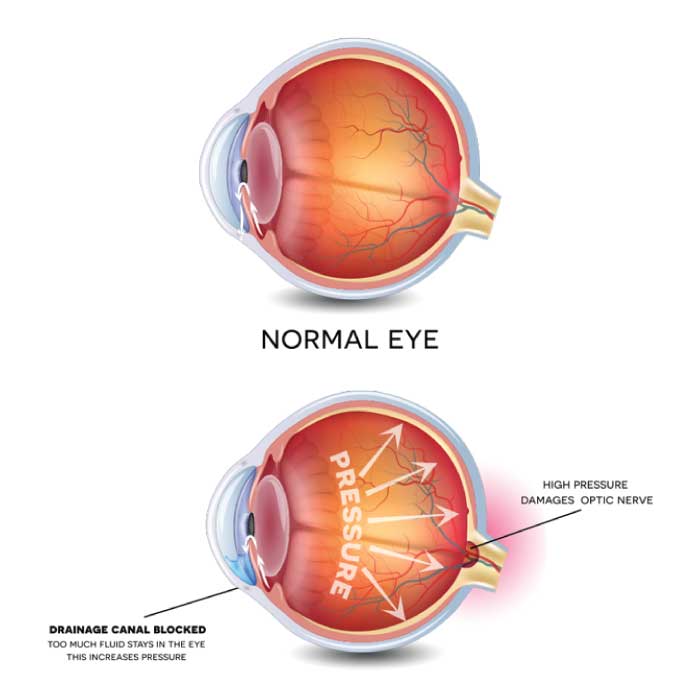
Glaucoma causes damage to the eye’s optic nerve and only worsens over time. Unfortunately, glaucoma has few or no initial symptoms. In most cases, it is associated with a higher-than-normal pressure inside the eye, but can also occur under normal intraocular conditions. If left untreated, glaucoma can cause peripheral vision loss and can eventually lead to blindness. Once detected, and dependent upon the severity, this disorder can be treated with either surgery, lasers, or medicated eye drops.
Cataracts
Cataracts, a clouding of the eye lens, can develop at any age, but they are commonly age-related and more prevalent in people aged 50 and older. Cataracts can be the result of injury or from protein deterioration causing the fluid inside the eyes lens to cloud. One of the primary causes of cataracts is believed to be prolonged exposure to UV (ultraviolet) light. If left untreated, cataracts can cause severe vision loss. The good news is that cataracts can be completely cured through surgery.
Diabetic Retinopathy
At first, unmanaged diabetes may not produce any noticeable symptoms. However, if diabetic retinopathy develops, it can cause changes in nearsightedness, farsightedness, and/or lead to blindness if left untreated. Many assume that a visit to a general practitioner is the only way to diagnose diabetes, but a comprehensive eye exam by an optometrist can lead to early detection of diabetes, reduce the risk of vision loss, and minimize the risk of developing other health complications.
Dry Eye Syndrome
Dry eye syndrome is when the eye does not produce tears properly, or when the tears are not of the correct consistency and evaporate too quickly. Lack of moisture causes inflammation of the surface of the eye. If left untreated, this condition can lead to pain, ulcers, or scars on the cornea, and in some rare cases, loss of vision. The good news is that it can often be treated with either over-the-counter or prescription eye drops, or rehabbing meibomian glands.

Amblyopia (Lazy Eye)
Amblyopia, also known as lazy eye, is a vision development disorder in which an eye fails to achieve normal visual acuity, even with prescription eyewear. Amblyopia begins during infancy and early childhood and often only affects one eye, but in some cases, reduced visual acuity can occur in both eyes. There are three types of amblyopia. Strabismic amblyopia is caused by the brain when it ignores the visual input from the misaligned eye in order to avoid double vision caused by poorly aligned eyes. Refractive amblyopia is caused by unequal refractive errors in the two eyes, despite perfect eye alignment. Deprivation amblyopia is caused by something like a cataract that obstructs light from entering and being focused in a baby's eye.
Amblyopia Symptoms, Causes & TreatmentAstigmatism
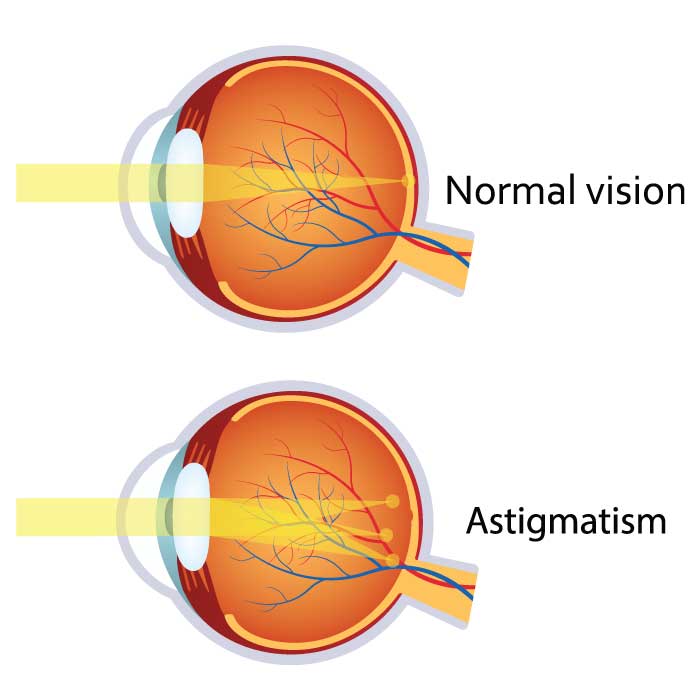
Like nearsightedness (i.e., myopia) and farsightedness (i.e., hyperopia), astigmatism is a refractive error, so it is an issue with how the eye focuses light, not an eye disease. In an eye with astigmatism, light fails to come to a single focus on the retina to produce clear vision. Instead, multiple focus points occur, either in front or behind the retina (or both). These multiple points of focus are typically caused by an irregularly shaped cornea. Instead of the cornea having a symmetrically round or spherical shape, it is more oval-shaped.
More About Astigmatism
Blepharitis
Blepharitis is inflammation of the eyelids in the areas where the eyelashes grow on both upper and lower eyelids. Blepharitis has two basic forms: anterior blepharitis, which affects the outside front of the eyelid where the eyelashes are attached, and posterior blepharitis, which is the result of dysfunctional meibomian glands, located within the eyelids, that secrete oils to lubricate the eye. It is common to experience a combination of both anterior and posterior forms of blepharitis at the same time. Blepharitis is often a chronic condition that is difficult to treat. However, although uncomfortable and unsightly, it is not contagious and usually cannot directly cause permanent damage to your eyesight, if properly treated.
Blepharitis Symptoms, Causes & TreatmentCataracts
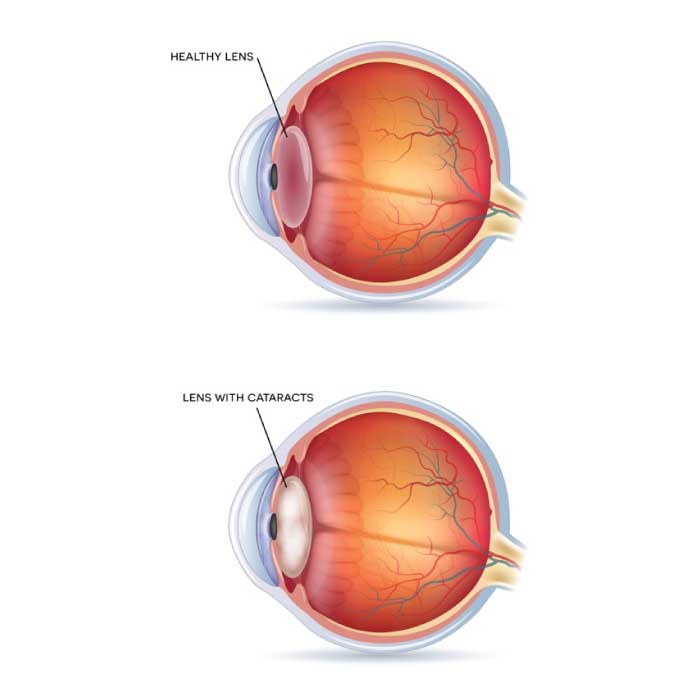
A cataract is a clouding of the eye's natural lens, which lies behind the iris and the pupil. Cataracts are the most common cause of vision loss in people over age 50 and they are the principal cause of blindness in the world. There are three types of cataracts: 1) a subcapsular cataract occurs at the back of the lens; 2) a nuclear cataract forms deep in the central zone (i.e., nucleus) of the lens; and 3) a cortical cataract occurs in the lens cortex, which is the part of the lens that surrounds the nucleus. Each type has its own unique symptoms.
Cataracts - Symptoms, Causes & Treatment
Chalazion / Stye
A chalazion is a small bump that appears on the eyelid because of a blocked oil gland. It’s similar to a stye (an enflamed oil gland on the eyelid), but is typically smaller and noticeably less painful. A chalazion can develop on the upper or lower lid, but often disappears without treatment in approximately 3-4 weeks.
Chalazion Symptoms, Causes & Treatment
Colour Blindness
Colour blindness, or colour vision deficiency (CVD), is the decreased ability to see colour or differences in colour. The most common form of colour blindness is known as red/green colour blindness. Individuals that suffer from red/green colour blindness tend to mix up all colours, which have a red or green components to their whole colour. Issues with discriminating between colours can arise across the entire colour spectrum and the effects can be mild, moderate or severe. Awareness is paramount to managing colour blindness because it allows the affected inividual, family and educators to adjust learning strategies accordingly.
Color Blindenss Symptoms, Causes & Treatment
Conjunctivitis (Pink Eye)
Commonly referred to as "pink eye", conjunctivitis is inflammation of conjunctiva, the thin, clear covering of the white of the eye, and the inside of the eyelids. Although the conjunctiva is transparent, it contains blood vessels that overlay the sclera of the eye. Inflammation will cause these conjunctival blood vessels to dilate. This is what causes red, bloodshot eyes. Conjunctivitis can have several causes but many eye doctors often use the term "pink eye" to refer only to viral conjunctivitis, a highly contagious infection caused by a variety of viruses. Conjunctivitis is a common eye problem that is easily treated and, with a few simple precautions like regularly hand washing, can often be avoided.
Conjunctivits (Pink Eye) Symptoms, Causes & Treatment
Corneal Abrasion
A corneal abrasion is simply a scratch on the cornea, the clear layer that covers the iris (i.e., the coloured part of your eye) and the pupil (i.e., the black circle in the centre of the eye). Corneal abrasions are one of the most common eye injuries. A scratched cornea often causes significant discomfort, redness, and hypersensitivity to light. In addition to impacting vision, a scratch on the cornea makes the eye susceptible to infection. Accordingly, treatment by an optometrist or ophthalmologist is often necessary.

Corneal Ulcer
A corneal ulcer is an open sore located on the cornea. Corneal ulcers are a serious condition and may result in loss of vision or blindness, if not properly treated. Most corneal ulcers are caused by bacterial infections. This is particularly common for contact lens wearers, who are highly susceptible to eye irritation. Viral (i.e. ocular herpes) and fungal infections can also lead to corneal ulcers, but are less common. Other underlying causes of corneal ulcers include dry eyes, allergies, and widespread general infection. Immune system disorders (e.g., multiple sclerosis) and inflammatory diseases (e.g., psoriasis) also can lead to corneal ulcers.
Detached Retina
A detached retina occurs when the retina becomes separated from its underlying supportive tissue. Flashes and floaters are common initial symptoms of a retinal detachment, or of a retinal tear that precedes the detachment itself. Because the retina cannot function when these layers are detached and because permanent vision loss may result if the retina is not immediately reattached, early detection and repair of retinal detachments is very important. The importance of early detection and treatment is further highlighted by the fact that visual improvement is much greater when the retina is repaired before the macula or central area is detached.
Retinal Detachment Symptoms, Causes & TreatmentDiabetic Retinopathy
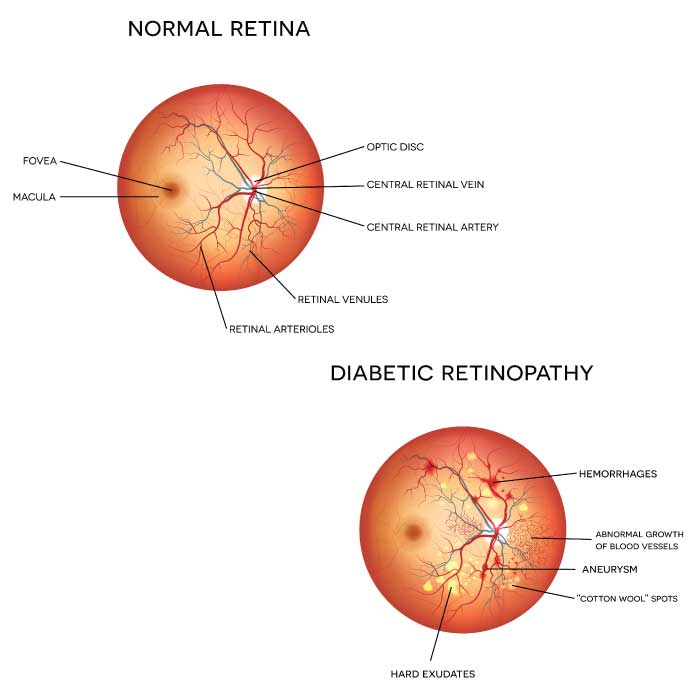
Diabetic retinopathy is a diabetes complication that affects the eyes. It's caused by damage to the blood vessels of the retina, the light-sensitive tissue at the back of the eye. This damage occurs when chronically high amounts of blood sugar begin to clog or damage blood vessels within the eye's retina, which contains light-sensitive cells (photoreceptors) necessary for good vision. In the early stages of diabetic retinopathy, blood vessel damage causes the retina to swell and form deposits. In later stages, leakage from blood vessels into the eye's clear, jelly-like vitreous can cause severe vision problems and may eventually lead to vision loss.
Diabetic Retinopathy Symptoms, Causes & Treatment
Diplopia (Double Vision)
Diplopia, commonly referred to as double-vision, is the simultaneous perception of two images of a single object. These images may be displaced horizontally, vertically, diagonally and/or rotationally in relation to each other. There are a number of possible medical reasons for chronic or frequent episodes of double vision. Some of these include stroke, head injury, brain tumour, brain swelling or brain aneurysm, corneal irregularities, dry eyes, or cataracts. However, the most common reason is impaired function of the extraocular muscles, where both eyes are still fully functional but cannot converge on the same desired object.

Dry Eye Syndrome
Dry eye syndrome (DES), also known as keratoconjunctivitis sicca (KCS), is the condition of having dry eyes. Dry eye occurs when either the eye does not produce enough tears or when the tears evaporate too quickly to properly and effectively lubricate and moisten the eye. Symptoms associated with dry eye syndrome include itching, burning, redness, photophobia, discharge, and easily fatigued eyes along with blurred vision, and can range from mild and occasional irritation to severe and continuous inflammation. While dry eyes are very common, and is a major reason why individuals visit their eye doctor, the symptoms can often be indicative of more serious ocular conditions.
Dry Eye Syndrome Symptoms, Causes & Treatment
Eye Herpes
Both types of herpes viruses, the varicella-zoster virus that causes causes chickenpox and shingles, and the herpes simplex type 1 virus that causes cold sores, can cause a condition called herpetic eye disease. When the former virus affects the eye, it is called herpes zoster ophthalmicus, and when the latter virus affects the eye it is referred to as herpes simplex keratitis. Both viruses can lead to corneal scarring and require immediate medical attention.

Eye Twitching
Eye twitching, eyelid tics, and spasms are common. With eye twitching, typically only the lower eyelid of one eye is involved, but the upper eyelid can also twitch. Eye twitching is often sporadic, but sometimes it can last for weeks or even months. Almost all sudden-onset eyelid twitching is benign, and not a sign of a medical problem. Often, a few lifestyle-related questions can help determine the likely cause of eye twitching and the best way to get it to stop. Stress and lack of sleep are the main culprits.
Floaters, Flashes, and Spots
Eye floaters are those tiny spots, specks, or flecks that appear to drift aimlessly around in your field of vision. Floaters and spots appear when tiny pieces of the eye's gel-like vitreous break loose within the inner back portion of the eye. While an annoyance, floaters and spots are common and typically aren't cause for concern. However, if you see a cloud of floaters and spots, especially if they are accompanied by flashes of light, you should seek medical attention immediately from an eye care professional. A sudden appearance of these symptoms could indicate that the vitreous is pulling away from your retina, or that the retina itself is becoming detached.
Glaucoma
Glaucoma refers to a group of related eye disorders that all cause damage to the optic nerve. This damage is most commonly caused by high pressure inside the eye (i.e., ocular hypertension) due to a buildup of excess fluid. Glaucoma initially causes loss of peripheral (side) vision, and if left untreated advances to later stages where central vision narrows to "tunnel" vision, often progressing until there is complete loss of vision. High eye pressure is not always a sign that an individual has glaucoma, but it is a strong indicator that one is at risk of developing it. Moreover, because glaucoma has few or no initial symptoms, early detection and treatment is essential to preventing severe vision loss or blindness.
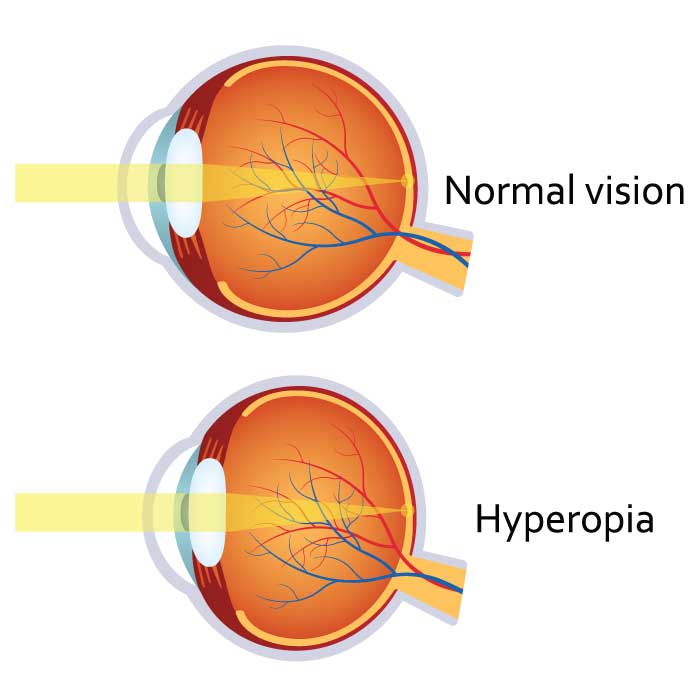
More About Glaucoma Glaucoma Symptoms, Causes & TreatmentHyperopia (Farsightedness)
Hyperopia, or farsightedness, is a common vision problem, affecting about one fourth of the population. People with hyperopia can see distant objects very well, but have difficulty focusing on objects that are up close. This vision problem occurs when light rays entering the eye focus behind the retina, rather than directly on it. The eyeball of a farsighted person is shorter than normal. This can be easily rectified through use of prescription eye glasses or contact lenses.
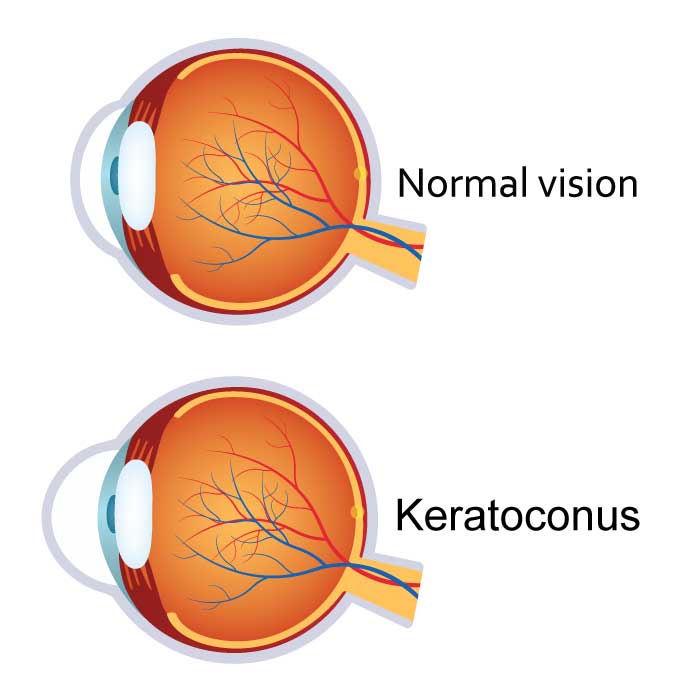
Keratoconus
Keratoconus is a degenerative disorder of the eye that causes the normally round cornea to thin and bulge into a more conical or cone-like shape. This cone shape deflects light as it enters the eye on its way to the retina, resulting in distorted vision. As the cornea becomes more conical in shape, it causes progressive nearsightedness and irregular astigmatism to develop, creating additional refractive errors that require more complex prescriptions. It also results in increased sensitivity to glare and light. Due to the progressive nature of keratoconus, patients with the disorder often require changes to their eyeglass prescription at every exam.
Keratoconus Symptoms, Causes & Treatment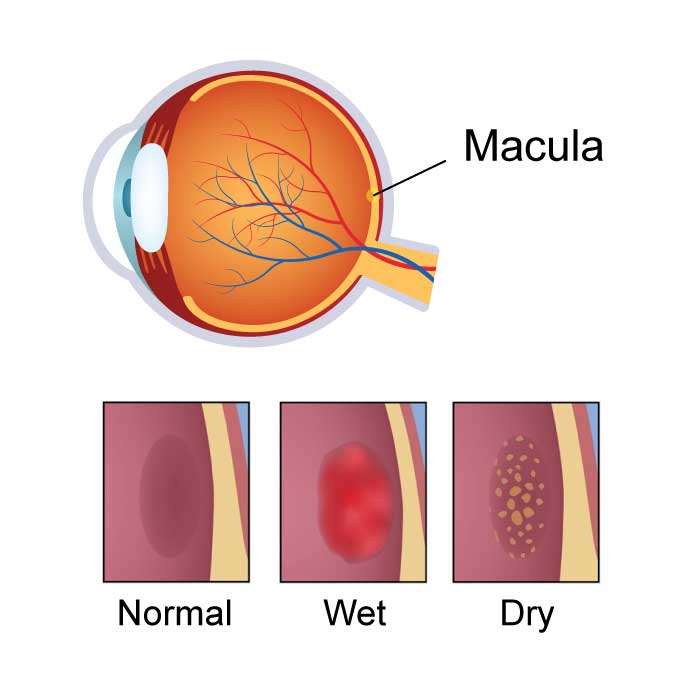
Macular Degeneration
Age-related macular degeneration — commonly shortened to macular degeneration, AMD or ARMD — is the deterioration of the macula, which is the small, central portion of the retina of the eye that influences and controls visual acuity. There are two types of macular degeneration, dry (non-neovascular) or wet (neovascular). Dry AMD is an early stage of the disease and is often the result of aging and thinning of macular tissues, deposits of pigment in the macula, or a combination of both. Wet AMD is the more advanced stage of the disease and is the more damaging form of the eye disease. With wet, or neovascular AMD, new blood vessels grow in the macula, where they are not intended to be. These new blood vessels grow beneath the retina and leak blood and fluid. This leakage causes permanent damage to the light-sensitive cells of the retina, which subsequently die off creating blind spots in central vision.
More About Macular Degeneration Age Related Macular Degeneration Symptoms, Causes & Treatment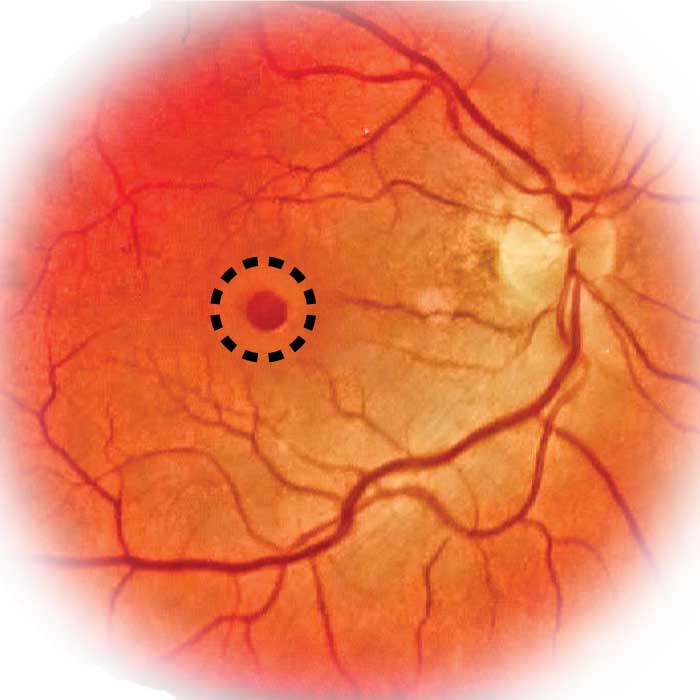
Macular Hole
A macular hole is simply a small break or hole in the macula, located in the centre of the eye's light-sensitive tissue called the retina. Because the macula is responsible for providing sharp central vision, a macular hole can result in extremely blurred or distorted central vision. How do macular holes typically occur? Most of the eye’s interior is filled with vitreous, a gel-like fluid that fills approximately 80 percent of the eye. The vitreous contains millions of fine fibres that are attached to the surface of the retina. As individuals age, the vitreous tends to slowly shrink and pull away from the surface of the retina. As this occurs natural fluids fill the void. This is normal and in most cases, there are no adverse effects. The exception is that some patients may experience a small increase in floaters. However, in some cases, the vitreous is firmly attached to the retina when it pulls away. This can tear the retina and create a macular hole. Moreover, when the vitreous pulls away from the surface of the retina, fibres can remain on the retinal surface and can contract. The resulting increased tension on the retina can also lead to the development of a macular hole. In both cases, the natural fluid that replaces the shrunk vitreous can then seep through the hole onto the macula, blurring and distorting central vision.
Myopia (Nearsightedness)
Myopia, or nearsightedness, is the most common refractive error of the eye, becoming increasingly more prevalent in recent years. A nearsighted individual typically will have difficulty reading traffic signs and seeing distant objects clearly, but will not have not issues with close-up tasks, such as reading or using a computer. Myopia occurs when the eyeball is too long relative to the focusing power of the cornea and lens of the eye. This causes light rays to focus at a point in front of the retina, rather than directly on its surface. Myopia can also be caused by the cornea and/or lens being too curved for the length of the eyeball. In some cases, nearsightedness is due to a combination of both conditions. This can be easily rectified through use of prescription eye glasses or contact lenses.

Ocular Migraine
Ocular migraines are painless, temporary visual disturbances that can affect one or both eyes. Although frightening and/or aggravating, ocular migraines are generally harmless and resolve themselves within 30 minutes. Individuals with ocular migraines can experience a variety of visual symptoms. Individuals may see a small, enlarging blind spot (scotoma) in their central vision with bright, flashing, or flickering lights (scintillations), or they may experience wavy or zig-zag lines surrounding the blind spot. In most cases, the temporary blind spot gradually enlarges and/or moves across the field of vision until it disappears.
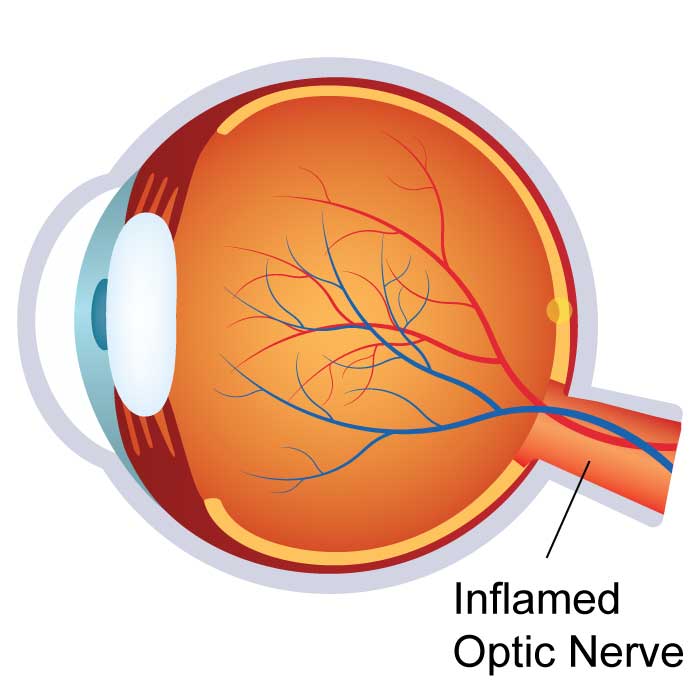
Optic Neuritis / Neuropathy
Optic neuritis is inflammation of the optic nerve, caused by damage to and loss of the protective sheath (myelin) surrounding the nerve. Individuals with optic neuritis often experience symptoms including blurred vision and blind spots. Individuals may also experience distorted vision, reduced colour vision, and pain when they move their eyes. It is noteworthy that these symptoms may precede vision loss due to optic neuritis. Optic neuritis is common with particular demographic segments and medical conditions. It commonly occurs in adults younger than 45 year of age and affects more women than men. The condition is also common for individuals with multiple sclerosis (MS), a condition that occurs when the body's own immune system attacks, damages, and destroys protective nerve coverings.
Optic Neuritis Symptoms, Causes & Treatment
Photophobia (Light Sensitivity)
Photophobia is an intolerance of, or sensitivity to light. Photophobia is not an eye disease, but rather a symptom of other conditions, such as infection or inflammation that can irritate the eyes. Light sensitivity can be a symptom of underlying conditions that don't directly affect the eyes, such as viral infections, severe headaches, or migraines. Other common causes of photophobia include corneal abrasion, uveitis, and central nervous system disorders, such as meningitis. Light sensitivity is also known to be the result of a detached retina, contact lens irritations, sunburn, and refractive surgery. In general, individuals with a lighter eye colour tend to experience more light sensitivity in bright environments because darker-coloured eyes contain more pigment to protect against harsh, direct lighting.

Pinguecula / Pterygium
A pterygium is an elevated, wedged-shaped bump on the eyeball that starts on the white of the eye (sclera) and can invade the cornea. A pterygium is a benign (non-cancerous) growth, but it can permanently disfigure the eye, cause discomfort, and blur vision. While it is widely agreed that ultraviolet radiation from the sun is the primary cause for their development and growth, dust, wind, and dry eye disease can also promote pterygia advancement.
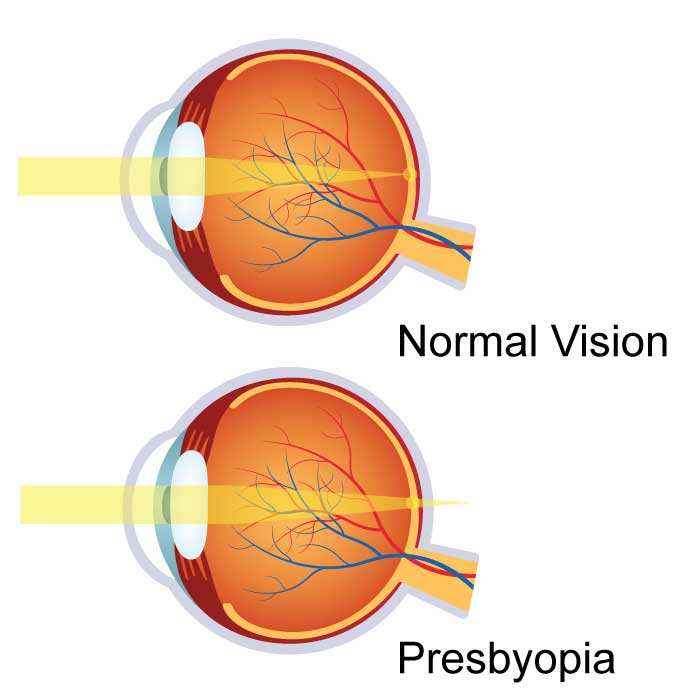
Pinguecula Symptoms, Causes & Treatment Pterygium Symptoms, Causes & TreatmentPresbyopia
Presbyopia is a condition that, sooner or later, affects the entire population. Individuals typically begin experiencing symptoms of presbyopia around age 40. The main symptom of presbyopia is blurred near vision when reading, writing, or working at the computer. Because natural physiological changes are the cause of presbyopia, individuals can't escape its affects, even if they have previously never experienced a vision problem. Moreover, even nearsighted individuals will notice that their near vision blurs when they wear their usual eyeglasses or contact lenses to correct distance vision. Signs and symptoms of individuals with developed presbyopia include the need to hold reading materials at arm's length in order to focus properly and experiencing headaches, eye strain, or feeling fatigued when performing near-distance work, such as sewing or handwriting.
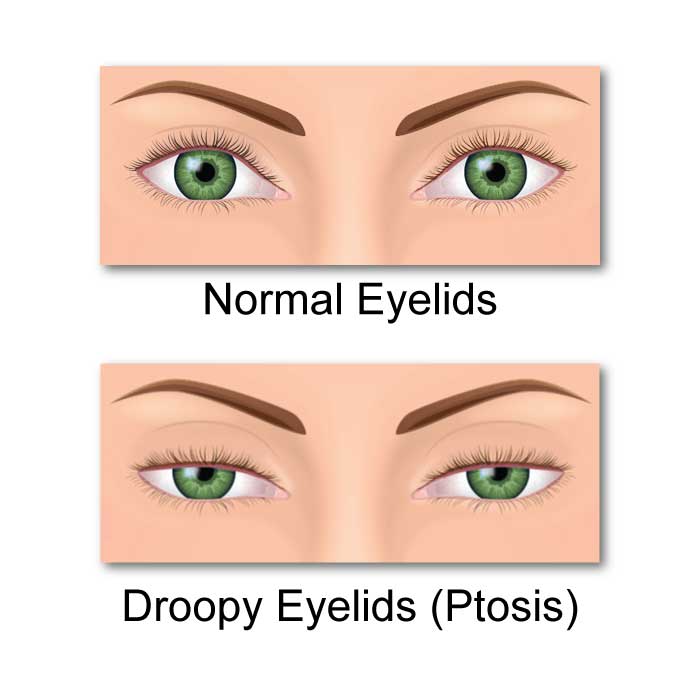
Ptosis (Drooping Eyelids)
Ptosis refers to drooping of the upper eyelid on one or both eyes. Ptosis can vary in severity from the droop being barely noticeable to the upper lid descending over the entire pupil. Ptosis can affect both children and adults, but is generally more common in individuals of advanced age. The most obvious sign of ptosis is the drooping eyelid. More subtle signs include individuals tilting their heads back in an attempt to see under the lid, or raising their eyebrows to try to lift the eyelid.
Ptosis Symptoms, Causes & Treatment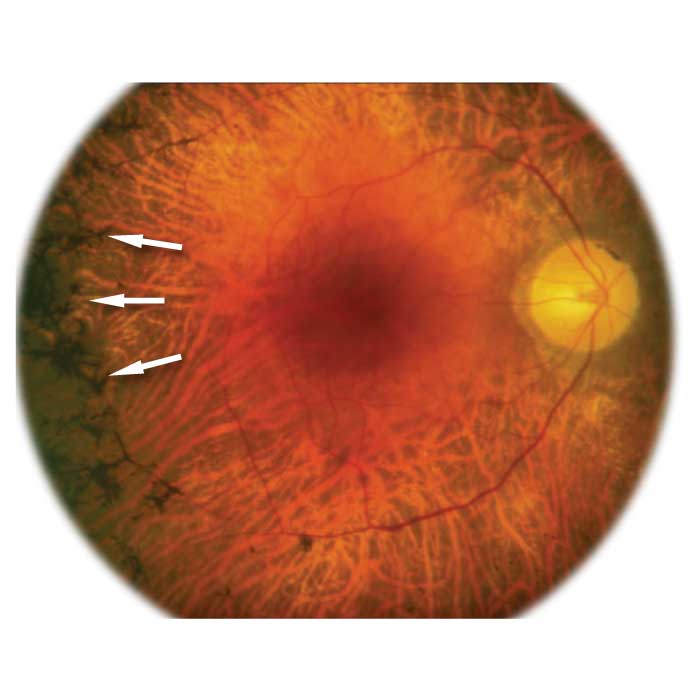
Retinitis Pigmentosa
Retinitis pigmentosa is a rare, inherited disease in which the retina slowly and progressively degenerates, eventually resulting in blindness. The first signs of retinitis pigmentosa usually occur in early childhood, when both eyes typically are affected. Symptoms also include poor night vision and a progressively narrowing field of vision.
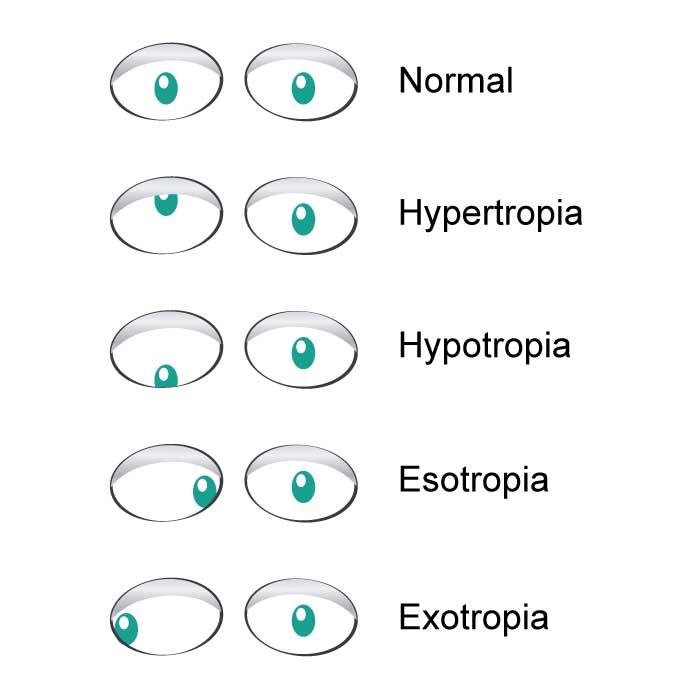
Strabismus
Strabismus is the failure of the eyes to maintain proper alignment, synchronization, and ability work together as a pair. When looking at an object, individuals with strabismus will have one eye looking directly at the object while the other eye is misaligned inward (esotropia, "crossed eyes" or "cross-eyed"), outward (exotropia or "wall-eyed"), upward (hypertropia), or downward (hypotropia). In addition to directional misalignment, symptoms of strabismus can vary temporally and in location. Strabismus can be constant or intermittent and misalignment may always affect the same eye (unilateral strabismus), or alternate between the two eyes (alternating strabismus). To prevent double vision from congenital and early childhood strabismus, the brain ignores the visual input from the misaligned eye, which typically leads to amblyopia or "lazy eye" in that eye. In most cases, strabismus and amblyopia can be successfully treated by eye training or surgery.
Strabismus Symptoms, Causes & Treatment
Subconjunctival Hemorrhage
A subconjunctival hemorrhage occurs when the small blood vessels beneath the tissue covering the white of the eye (conjunctiva) break, causing eye redness. A subconjunctival hemorrhage is often benign, causing no vision impairment or significant eye discomfort despite its seemingly painful appearance. However, conjunctiva redness can also be a sign of several potentially serious eye conditions. In cases where eye discharge coincides with conjunctiva redness, individuals should see an optometrist for an eye exam to rule out an infection caused by bacteria, virus, or microorganism.

Uveitis
Uveitis is inflammation of the uvea — the middle layer of the eye that consists of the iris, ciliary body, and choroid. Eye injuries, inflammatory diseases and exposure to toxic chemicals, like pesticides and acids used in manufacturing processes, can cause uveitis. For many, uveitis is a chronic condition that can potentially produce a number of complications, including a clouding of the cornea, cataracts, elevated eye pressure, glaucoma, swelling of the retina, or retinal detachment. All of these complications can result in permanent vision loss.
Uveitis Symptoms, Causes & Treatment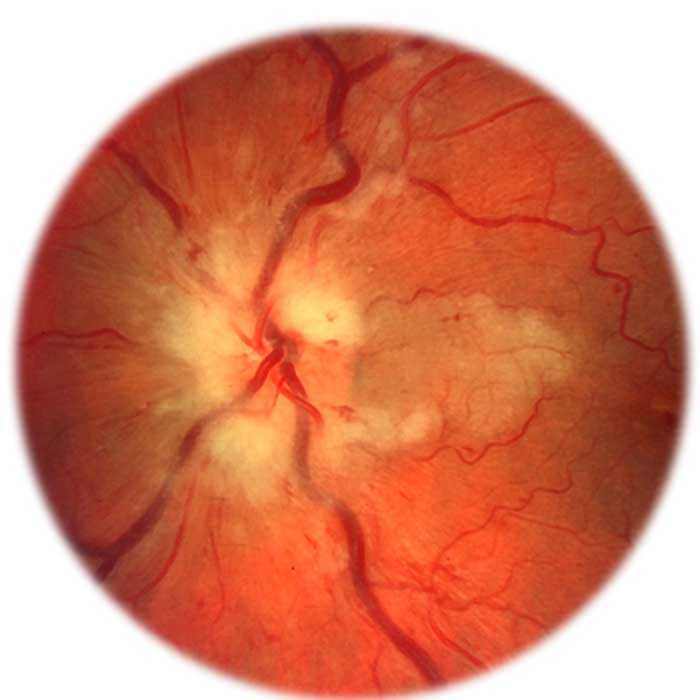
Vascular Occlusions (Eye Strokes)
Eye strokes occur when blockages (occlusions) occur in arteries or veins in the retina, causing vision loss. The severity of vision loss largely depends on the extent and location of the occlusion(s) and loss of blood flow. Similar to when strokes occur in other parts of the body when blood flow is blocked, the eye may suffer irreparable damage when the retina and/or optic nerve are cut off from nutrients and oxygen supplied by the flow of blood via the circulatory system.
Our Edmonton Optometrists
Searching for an optometrist in Edmonton? Our experienced Edmonton eye doctors use advanced modern technologies and devote upwards of 500% more time towards providing personalized patient care than elsewhere so that they can see more and ensure that you may never see less. Position yourself to see the future with a visit to our eye clinic and Edmonton's best eye care!

Dr. Jennifer Ash, OD
Dr. Jennifer Ash is the Resident Optometrist at Eye-deology Vision Care. Dr. Ash provides patient care 5 days a week. Read more about Dr. Ash.

Dr. Ruhee Kurji, OD
Dr. Ruhee Kurji is an Associate Optometrist at Eye-deology Vision Care. Dr. Kurji provides patient care Tuesdays & Fridays. Read more about Dr. Kurji.

Dr. Jade McLachlin, OD
Dr. Jade McLachlin is an Associate Optometrist at Eye-deology Vision Care. Dr. McLachlin provides patient care 5 days a week. Read more about Dr. McLachlin.

Dr. Tania Mathews, OD
Dr. Tania Mathews is an Associate Optometrist at Eye-deology Vision Care. Dr. Mathews provides patient care 2 days a week. Read more about Dr. Mathews.
Learn Why Our Edmonton Optometrists Are The Best!